Cannabis Withdrawal Syndrome Timeline: Day-by-Day Symptom Map
Withdrawal & Recovery
Days 2-6 Peak
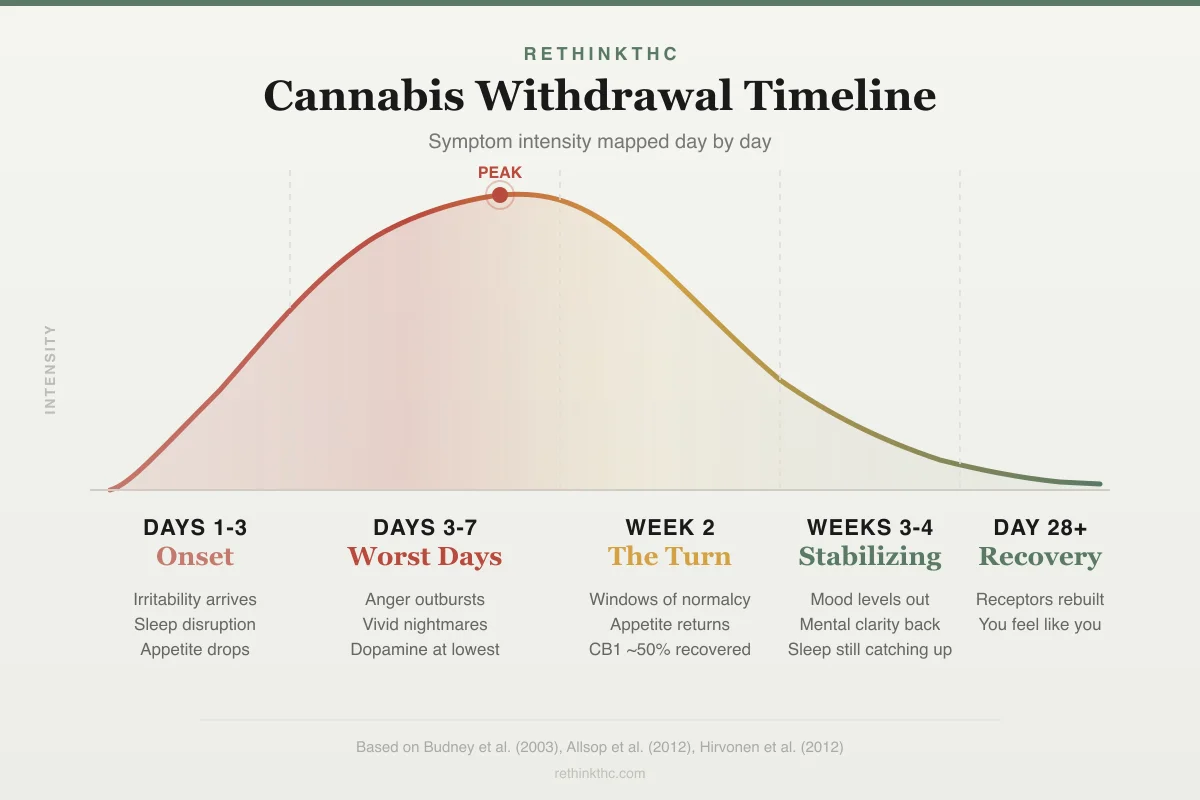
Two controlled studies converged on the same withdrawal arc — onset days 1 to 3, peak days 2 to 6, near-normal by week 4 — driven by CB1 receptor recovery that begins within 48 hours.
Journal of Abnormal Psychology, 2003
Journal of Abnormal Psychology, 2003
 View as image
View as imageCannabis withdrawal syndrome unfolds on a biological timetable that research has now mapped in considerable detail. That timetable is the subject of this article. Rather than a general overview of what withdrawal feels like, this is a phase-by-phase breakdown that tells you which symptoms are most active on which days, what is driving them at a neurological level, and what is actually useful to do in each window. The research behind this timeline comes primarily from two well-controlled studies: Budney et al. (2003), published in the Journal of Abnormal Psychology,[1] which followed 18 frequent cannabis users under controlled conditions over 50 days, and Allsop et al. (2012), published in PLOS ONE,[2] which validated the timeline across 49 cannabis-dependent participants. Both converged on the same arc.
For a full overview of the syndrome itself, including the DSM-5 criteria and the neuroscience of why withdrawal exists, see the complete guide to cannabis withdrawal. For a clinical deep dive into the diagnostic criteria specifically, see cannabis withdrawal syndrome DSM-5.
Key Takeaways
- Cannabis withdrawal follows a predictable schedule: onset days 1 to 3, peak days 2 to 6, big improvement by week 2, and near-normal by weeks 3 to 4
- That timing is driven by CB1 receptor recovery in your brain, which kicks in within 2 days and largely wraps up around day 28
- Different symptoms hit at different phases — irritability and insomnia come first, mood and appetite problems peak around days 3 to 7, and sleep is the last thing to fully normalize
- Knowing which phase you are in makes each stage easier to ride out, because you are watching a known process instead of wondering if something is wrong
- This timeline is built on two controlled studies that tracked real withdrawal under documented conditions — not just self-report surveys
- Your personal timeline shifts based on how often and how long you used, product potency, tobacco use, sex differences, and whether you quit cold turkey or tapered
The Biological Clock Behind the Timeline
Before going day by day, it helps to understand what drives the timing in the first place. When you use cannabis regularly, your brain reduces the number and sensitivity of CB1 receptors, which are the docking sites in your brain where THC produces its effects. This process, called downregulation, happens across brain regions that govern mood, sleep, appetite, stress response, and temperature regulation.
When you stop, THC disappears from your system, but your receptor population has not yet recovered. The gap between what your brain is used to having available and what it actually has is what generates withdrawal symptoms. The symptoms resolve as the receptors rebuild.
Research published in Molecular Psychiatry in 2012[3] used brain imaging to track this recovery directly and found that CB1 receptors begin rebuilding within approximately two days of stopping cannabis. Research published in Biological Psychiatry in 2016[4] confirmed that the recovery process is underway from the very first days of abstinence and continues progressively until receptor density approaches normal levels at around day 28. That 28-day window is the biological clock driving the entire timeline below.
Days 1 to 3: Onset
Cannabis Withdrawal: Day-by-Day Map
What You Feel
Day one is often quieter than people expect. You may feel a faint restlessness or an edge to your mood, but the more dramatic symptoms have not arrived yet. Some people feel essentially nothing on day one and wonder if they are going to be one of the lucky ones who skips withdrawal. That mild start reflects the fact that THC is fat-soluble and stored in body fat. For the first 24 hours, significant THC is still being released from storage into your bloodstream, so your brain has not fully registered the absence.
By days two and three, the shift is noticeable. Irritability arrives first, often sharply. You may snap at someone and immediately recognize that your reaction was disproportionate. Sleep becomes difficult: falling asleep takes longer, you wake during the night, and the sleep you do get feels shallow. Appetite drops. The thought of eating is either uninteresting or actively unappealing. Budney et al. (2003)[1] found that irritability and sleep disturbance are typically the first symptoms to reach clinical significance, most commonly emerging by day two.
Physical symptoms can begin here, though they are usually not at peak intensity yet. Mild headaches, a general feeling of being physically off, and for some people, mild nausea or stomach discomfort. Cannabis withdrawal syndrome recognized in the DSM-5 specifically includes these physical symptoms alongside the psychological ones, so if you feel physically unwell, that is part of the documented picture.
Cravings may also appear in this window. These are not purely psychological. Your brain's reward circuitry has learned to expect THC at certain times and in certain situations, and the absence of the expected signal generates a real neurological response.
What Is Happening Neurologically
Your CB1 receptors are just beginning to register the sustained absence of THC. The endocannabinoid system, which normally helps regulate all the functions that are now starting to feel disrupted, is running below capacity because its external support has been removed and its internal production machinery has been in reduced operation. Research by D'Souza and colleagues[4] confirms that receptor recovery does begin within these first two days, but it is just starting. The gap between demand and capacity is at its widest during this early phase.
What Actually Helps
Use the relative calm of day one to set up your environment. Stock food you can eat with minimal appetite (crackers, fruit, simple soups). Arrange your sleep space: cool room, dark curtains, no screens in the hour before bed. Tell one person you trust what you are doing, not for accountability, but so that someone around you understands why you might seem irritable over the coming week.
When cravings arrive, use the 15-minute rule. Each craving peaks and fades within approximately 15 to 20 minutes. You do not need to resist indefinitely. You just need to get through the next 15 minutes. Walking during a craving is particularly effective because physical movement activates your brain's own endocannabinoid production, providing some natural replacement for what THC was doing.
Days 3 to 7: Peak Intensity
What You Feel
This is the hardest part of the timeline. Budney et al. (2003)[1] documented that withdrawal symptoms peak between days two and six, and Allsop et al. (2012)[2] confirmed the same window across their sample. If you are reading this from inside days three through seven, you are at the worst point. It does improve from here.
Irritability during peak can feel volcanic. Anger outbursts are common, particularly when frustrated or sleep-deprived. Allsop et al. specifically identified angry outbursts as among the most impairing symptoms their participants reported. Sleep disruption is typically at its most severe: many people get only a few broken hours per night during this window. When you do sleep, dreams become vivid, intense, and sometimes disturbing. This is REM rebound. THC suppresses the dreaming stage of sleep, so when THC is removed, your brain floods you with dreaming sleep to compensate. The nightmares can be jarring if you do not know that is what is happening. For a detailed look at this specific phenomenon, see nightmares after quitting weed.
Mood swings during peak phase are significant. You might feel okay for a stretch and then be hit with a wave of sadness, flat affect, or anxiety that seems to come from nowhere. Anxiety during weed withdrawal is one of the most consistently reported symptoms in this phase. Concentration is poor. Nothing feels interesting or rewarding. Some people describe a gray quality to experience during this phase, where activities they normally enjoy feel flat or pointless. Night sweats and physical discomfort, including shakiness or stomach cramping, may intensify.
Appetite may be substantially suppressed. Some people lose several pounds during the first week from the combined effects of reduced appetite and poor sleep.
What Is Happening Neurologically
Your CB1 receptor population is in its most active phase of rebuilding, but is still well below normal density. The brain regions most affected include the amygdala (the area that processes threat and emotional reactivity), which is running without its normal dampening input from the endocannabinoid system. This is why emotions feel disproportionate and why the stress response is heightened. Your brain is not broken. It is operating without the regulatory cushion it has been accustomed to, and it is overcorrecting before it stabilizes.
Dopamine levels are also at their lowest point during this window. THC artificially elevated dopamine each time you used. Without that boost, dopamine falls below your natural baseline before your system recalibrates. This is why nothing feels interesting or rewarding right now. Your dopamine system is recovering, not permanently impaired. See dopamine recovery after quitting weed for a full account of this process.
Irritability during this phase has a direct neurological basis. For a detailed breakdown of why anger and irritability hit so hard and what helps, see anger and irritability quitting weed.
What Actually Helps
The goal during peak is not optimization. It is survival. Do not make major decisions during days three through seven. Do not try to evaluate your long-term mental health based on how you feel right now. Do not judge your natural personality by your current irritability. You are running on depleted neurochemistry. This is temporary.
Exercise remains the most reliably effective intervention. Even a 20-minute walk measurably shifts endorphins and promotes endocannabinoid production. On the days when you feel worst, the walk will not feel good beforehand, but it will feel better during and after. Eat small meals regularly even without hunger. Your brain needs glucose and micronutrients to rebuild receptor infrastructure. Dehydration makes headaches and irritability significantly worse, so keep fluids up.
For insomnia, avoid lying in bed frustrated for extended periods. If you are not asleep within 30 minutes, get up, do something boring in dim light (reading a physical book, sitting quietly), and return to bed when you feel sleepy again. This preserves the association between bed and sleep rather than bed and frustrated wakefulness. For a detailed look at managing sleep during this phase, see weed withdrawal insomnia and how to sleep without weed.
Week 2: The Turn Begins
What You Feel
Somewhere in the second week, something shifts. The change is gradual, not dramatic, but it is real. Irritability loses its sharp edge. Cravings come less frequently and feel more like suggestions than demands. Appetite begins returning, sometimes as hunger for specific foods rather than general appetite. You may wake up actually hungry for the first time in a week.
Sleep is still disrupted but improving. You are logging more total hours. Vivid dreams continue and can remain intense, but the overall picture is moving in a better direction. The most distinctive marker of week two is the appearance of windows: stretches of time, sometimes an hour or two, sometimes longer, where you feel genuinely like yourself. Normal. These windows are significant. They are evidence that your brain is recovering, and they get longer and more frequent as week two progresses.
Mood is less volatile. You can sit through a conversation or a frustrating situation without the reactive edge of peak phase. Some people begin noticing small pleasures returning, brief moments of genuine enjoyment that were absent during days three through seven. The gray quality starts to lift.
What Is Happening Neurologically
By day 14, your CB1 receptor density has recovered to roughly 50 to 60 percent of its normal level based on the neuroimaging data from the 2012 study[3]. That is meaningfully better than the depleted state of peak withdrawal, though still below the normal baseline your brain is working toward. Endocannabinoid production is increasing. The gap that drives withdrawal is narrowing.
Your dopamine system is also recovering. Neurotransmitter levels are approaching your natural baseline, which is why brief periods of normal reward and pleasure are starting to break through. First week quitting weed puts this turning point in context with what preceded it.
What Actually Helps
Start tracking your symptoms day by day if you have not already. A simple note of how you felt, even just a few words, creates a record that shows you the trajectory. It is very hard to notice gradual improvement from inside it. A record from day four that says "brutal, no sleep, angry at everything" makes your day twelve feel like measurable progress.
Reintroduce activities you used to enjoy, even if they feel slightly flat compared to how they felt when you were using. This is expected, and it resolves as your dopamine system continues recovering. The mild flatness you feel is not permanent. It is your brain still calibrating.
Nutritional support during this phase can help. Several nutrients support neurotransmitter synthesis and receptor function. For an evidence-based look at what helps, see supplements for weed withdrawal.
Weeks 3 to 4: Normalization
What You Feel
Most of the acute withdrawal picture has resolved by weeks three and four. Mood is substantially more stable. Concentration is returning. You can handle frustration, difficult situations, and everyday stress without the volatility of the peak phase. Appetite is back to normal, and many people notice they are genuinely hungry with preferences and enjoyment of food rather than just eating because they need to.
Cognitive function improves noticeably during this period. Working memory, processing speed, and the ability to focus on a task for sustained periods all get measurably better. Many people describe a mental sharpness during this phase that surprises them, a sense of being more present and clear-headed than they realized was possible.
Sleep is still the holdout. Clinical research has documented that sleep disturbances can persist for 40 to 45 days after stopping cannabis. By weeks three and four, sleep is likely notably better than it was, but it may not yet feel fully normal. Vivid dreams continue for many people into week four, though with less intensity than in the acute phase. Night sweats, if present earlier, have typically resolved by now.
Cravings are situational rather than constant. They surface in specific contexts, particular times of day, social settings, or stress responses that previously signaled cannabis use. This is expected. The neural pathways that associated those situations with cannabis are still intact and will fade gradually with time.
What Is Happening Neurologically
CB1 receptor density is approaching normal levels. The 2012 study[3] and the 2016 research[4] converge on approximately day 28 as the point when receptor recovery reaches near-normal levels. Your endocannabinoid system is largely self-sufficient again. The emotional regulation systems in your prefrontal cortex (the brain region responsible for planning, decision-making, and moderating impulses) are operating more reliably. The amygdala's reactivity is settling down as the regulatory input from a recovered endocannabinoid system returns.
The sleep system is the last to complete its reorganization. THC profoundly alters sleep architecture, particularly suppressing REM sleep. Your brain is in the final stages of restoring normal REM and deep sleep ratios, which is why sleep improvements during weeks three and four are real but still incomplete. For a detailed look at what is happening with your sleep at this stage and what the research says about REM recovery, see THC and REM sleep rebound.
What Actually Helps
This phase is where the work of building new patterns pays off. Cravings are now predictable enough that you can develop specific responses to specific triggers. If you notice a craving at 9 pm when you used to smoke, having an alternative activity planned for that exact time changes the neurological association over time.
Physical exercise continues to be the most effective non-pharmaceutical support for dopamine recovery and sleep normalization. Consistent sleep and wake times during this phase, even on weekends, help your circadian rhythm complete its reset. Avoid caffeine after noon. Keep your sleep environment consistent.
This is also a good window to examine what role cannabis was playing in your life before you stopped. If you were using it heavily to manage anxiety, and anxiety is still present now in a milder form, that anxiety may benefit from its own targeted approach. See managing anxiety without weed and the anxiety toolkit for weed withdrawal.
Beyond Day 28: Post-Acute Phase
For most people, the acute withdrawal syndrome is largely resolved by day 28 to 45. CB1 receptors are at or near normal density. Endocannabinoid function is restored. The biological basis for withdrawal symptoms has cleared.
A subset of heavy, long-term users, particularly those who used daily for years with high-potency products like concentrates or high-THC vape cartridges, may notice milder residual effects that persist beyond the acute window. These might include occasional low-motivation days, brief mood dips, or intermittent sleep disruption. These are significantly less disruptive than the acute phase and follow a continuing trajectory of gradual improvement. Researchers sometimes call this post-acute withdrawal syndrome (PAWS), though it is not a formally recognized separate diagnosis in cannabis. For more on what this phase looks like and how long it may last, see PAWS and cannabis post-acute withdrawal and how long to feel normal after quitting weed.
The most important thing about the post-acute phase is the direction. Each week is better than the last, even when the improvement is subtle enough to only notice in retrospect.
What Shapes Your Personal Timeline
The timeline above reflects the average across clinical research populations. Several factors push your experience earlier, later, more intense, or more mild.
Frequency and duration. Daily use over years produces more thorough neurological adaptation than daily use over months, which produces more than occasional use. More thorough adaptation means a wider gap to close when you stop, and a slightly longer timeline to full normalization. For a detailed look at all the factors that affect your personal timeline, see how long does weed withdrawal last.
Product potency. Concentrates, dabs, and high-THC vape cartridges deliver dramatically more THC per session than traditional flower. Users of high-potency products tend to experience more pronounced CB1 downregulation and can expect a more intense and potentially longer acute withdrawal period.
Concurrent tobacco use. If you smoked blunts or mixed cannabis with tobacco, nicotine withdrawal may run alongside cannabis withdrawal. Nicotine withdrawal has its own symptom profile (irritability, difficulty concentrating, craving) that overlaps with cannabis withdrawal and can amplify the overall intensity.
Sex differences. Research suggests that women may process THC differently and experience some withdrawal symptoms with different intensity patterns. See weed withdrawal in women for the specific research on sex differences in cannabis withdrawal.
Method of quitting. Whether you stop all at once or taper down affects the acute intensity of the first few days. For a detailed look at both approaches and what the evidence says about their outcomes, see cold turkey vs. taper quitting weed.
When to Seek Professional Help
Cannabis withdrawal syndrome is uncomfortable, sometimes significantly so, but it is not medically dangerous in the way that alcohol or benzodiazepine withdrawal can be. Most people move through it without formal medical support.
That said, seek professional support if insomnia has not meaningfully improved by week six, if anxiety or depression during withdrawal is severe enough to interfere with your ability to work or care for yourself, if you are experiencing any thoughts of self-harm, or if you have tried to quit multiple times and withdrawal symptoms consistently drive you back before you can stabilize. A clinician can assess whether your symptoms are fully explained by withdrawal or whether an underlying condition needs independent treatment.
SAMHSA's National Helpline is available at 1-800-662-4357. It is free, confidential, and available 24 hours a day, 7 days a week. You can also text "HELLO" to 741741 to reach the Crisis Text Line.
The Bottom Line
Cannabis withdrawal syndrome follows a predictable biological schedule driven by CB1 receptor recovery. Symptoms onset days 1 to 3 (irritability and insomnia arrive first), peak days 2 to 6 (mood volatility, appetite suppression, vivid dreams, physical discomfort at maximum intensity), improve significantly by week 2 (windows of normalcy appear), and approach normalization by weeks 3 to 4 (CB1 receptors reach near-normal density around day 28). Sleep disturbance is the longest-lasting symptom, persisting up to 40 to 45 days. The timeline is based on controlled studies by Budney et al. (2003) and Allsop et al. (2012), with the biological mechanism confirmed by PET neuroimaging showing CB1 receptor recovery beginning within 2 days and largely completing by day 28. Individual timelines vary based on usage history, product potency, concurrent tobacco use, and quitting method.
Frequently Asked Questions
Sources & References
- 1RTHC-00134·Budney, Alan J. et al. (2003). “When Heavy Users Quit Cannabis, Symptoms Show Up Fast and Ease Within Two Weeks.” Journal of Abnormal Psychology.Study breakdown →PubMed →↩
- 2RTHC-00538·Allsop, David J. et al. (2012). “Withdrawal That Disrupted Daily Life Was Tied to Relapse in a Small Study.” PLOS ONE.Study breakdown →PubMed →↩
- 3RTHC-00573·Hirvonen, Jussi et al. (2012). “Daily Cannabis Use Was Linked to Fewer CB1 Receptors. A Month Without Brought Them Back..” Molecular Psychiatry.Study breakdown →PubMed →↩
- 4RTHC-01134·D'Souza, Deepak Cyril et al. (2016). “Brain Cannabinoid Receptors Drop With Heavy Use, Then Rebound Within Days of Stopping.” Biological Psychiatry: Cognitive Neuroscience and Neuroimaging.Study breakdown →PubMed →↩
Research Behind This Article
Showing the 8 most relevant studies from our research database.
Prevalence of cannabis withdrawal symptoms among people with regular or dependent use of cannabinoids: A systematic review and meta-analysis
Bahji, Anees · 2020
This was the first meta-analysis to estimate how common cannabis withdrawal syndrome actually is.
Cannabinoid Hyperemesis Syndrome: Diagnosis, Pathophysiology, and Treatment-a Systematic Review.
Sorensen, Cecilia J · 2017
This extensive systematic review analyzed 2,178 articles, ultimately including 183 studies with cumulative case data.
Varenicline for cannabis use disorder: A randomized controlled trial.
McRae-Clark, Aimee L · 2026
Varenicline did not reduce cannabis use sessions overall during weeks 6-12.
Rural and Urban Variation in Mobile Health Substance Use Disorder Treatment Mechanisms and Efficacy.
Mennis, Jeremy · 2026
The PNC-txt mobile health intervention reduced cannabis use at 6 months by increasing readiness to change and protective behavioral strategies at 1 month.
Nabiximols as an agonist replacement therapy during cannabis withdrawal: a randomized clinical trial.
Allsop, David J · 2014
In a double-blind clinical trial, 51 cannabis-dependent treatment seekers received either nabiximols (up to 86.4 mg THC and 80 mg CBD daily) or placebo during a 9-day inpatient admission, followed by 28 days of outpatient follow-up.
Cannabis Withdrawal and Psychiatric Intensive Care.
Malik, Aliyah · 2025
Among 52,088 psychiatric admissions in London over 16 years, cannabis users were 44% more likely than non-users to require psychiatric intensive care overall.
Cannabis withdrawal in the United States: results from NESARC.
Hasin, Deborah S · 2008
Using data from the National Epidemiologic Survey on Alcohol and Related Conditions (NESARC), researchers examined cannabis withdrawal among 2,613 frequent users (three or more times per week) and a subset of 1,119 "cannabis-only" users who didn't binge drink or use other drugs frequently. Withdrawal was common: 44.3% of the full sample and 44.2% of the cannabis-only subset experienced two or more symptoms.
The cannabis withdrawal syndrome: current insights.
Bonnet, Udo · 2017
The review synthesized evidence that regular cannabis use causes desensitization and downregulation of brain CB1 receptors, which begins reversing within the first 2 days of abstinence and normalizes within about 4 weeks.